Innovations for Maternal, Newborn & Child Health
Funded by the Bill and Melinda Gates Foundation, this program applied design thinking to improve the lives of the world’s most vulnerable women and children.
PLEASE NOTE: THIS A LEGACY PROGRAM AND NO LONGER ACTIVE
The Challenge
Every year, nearly 6 million children die before their fifth birthday. Most of these deaths occur in low-income countries, where health systems are more likely to be weak. And most of these deaths are the result of easily preventable and treatable illnesses, including malaria, diarrhea, and respiratory infections (often further complicated by malnutrition).
There is also a large overlap between countries where infant mortality rates are high and countries where maternal mortality rates are high. For 300,000 women each year, pregnancy and childbirth are a death sentence, and options for quality prenatal healthcare are few and far between. Remote locations, social structures, conflict, and instability make it difficult for many women to seek care.
The question: could design thinking help find creative solutions to maternal and child mortality rates?
Designing a Solution for Prenatal Growth
Funded by the Bill & Melinda Gates Foundation, Concern Worldwide launched Innovations for Maternal, Newborn & Child Health to develop and test creative solutions to this challenge using design thinking.
A popular method in technology and the for-profit sector, design thinking is a process that places the people for whom a product or program is being developed at the heart of the process. The system revolves around understanding the user, challenging assumptions, and redefining problems in order to find innovative solutions that get to the heart of an issue. Or, as Jeanne Ledtka wrote in the Harvard Business Review, “It addresses the biases and behaviors that hamper innovation.” When the system works, it means that the solutions are more sustainable and more likely to be widely adopted, because they meet the needs of the user rather than the goals of the creator.
At Concern, where we have spent the last 50+ years placing local knowledge and expertise at the center of our programs and work to understand communities’ needs, experiences, and goals, this process seemed like a natural fit.

What We Mean By Innovation
Innovations for Maternal, Newborn, and Child Health tested a hypothesis: Could we center marginalized voices — people who have never been heard, but who live with these challenges on a daily basis — and crowdsource groundbreaking solutions?
Concern embarked on this work in 2009, guided by five core principles:
- Commit to source and refine ideas in new, unconventional ways
- Take risks — one of the biggest risks being this untested crowdsourcing method
- Evaluate rigorously and document our findings robustly
- Accept that not every innovation would succeed
- Work to ensure that the successful innovations would be sustained and scaled
Today, “innovation” is a popular buzzword. But in 2008, when we put this project proposal together, it was more unusual, especially in our area of work. The Bill and Melinda Gates Foundation was also much younger as an organization, and had just completed its first maternal, newborn, and child health project before funding Concern’s. This work was therefore taken on in the spirit of co-creation and shared learning.
Finding Ideas
Guided by the work of organizations such as IDEO, Ashoka Changemakers, and the IBM Innovation Jam, Concern began by sourcing ideas in Malawi, Sierra Leone, and India. Between 2009 and 2010, we conducted extensive research to understand the clear, specific problems affecting maternal and child health coverage, access, and mortality. We then put out calls and contests for proposals.
In all, we received 12,762 proposals, and evaluated them based on how much they represented previously unheard voices, the problems they addressed, and the characteristics of the solutions. In Malawi alone, we received 6,112 proposals. 53% addressed facility-level solutions, 14% addressed community-based solutions, and 26% addressed government or health systems solutions.

Putting Ideas Into Action
In 2011, Innovations began implementing some of the winning proposals in Malawi, Sierra Leone, and India. Working closely with local partners, we designed evaluations, gathered baseline data, and started generating evidence on processes and outcomes.
Concern successfully brought nine projects through rigorous testing, development, and evaluation with innovations.
By the end of that year, we’d found a solid structure for incubating these projects and working with design thinking to evaluate, adapt, and refine processes and projects. We also realized that we could cluster separate ideas and projects together to form a cohesive whole, which benefited everyone involved. Phase Two of Innovations launched in 2012, along with more pilots of solutions in Kenya, Sierra Leone, and Ghana. All pilots ran for at least 18 months, with the final projects concluding at the end of 2016.
At the end of an eight-year project, Concern had successfully brought nine projects through rigorous testing, development, and evaluation. Which begged the question: What is “innovation,” especially in terms of humanitarian aid and development?
Innovations director Pat Dandonoli considered this question halfway through our project, in 2012:
"An entire industry is forming around methods and toolkits for promoting, fostering, and designing innovation, implying that anyone, armed with some sticky notes, can innovate. Truly transformative innovation is rare and there are many routes to achieving it."
Through this project, we didn’t get to any fail-proof recipe for innovation. But that makes sense: If there was a “magic bullet” technique for solving all of the issues behind poverty, we’d be out of business already. But the power of authentic, empathic engagement was a key ingredient in the solutions that worked.

What Projects Came Out Of Innovations?
Malawi: Chipatala Cha Pa Foni
Chipatala Cha Pa Foni, or Health Center by Phone, was designed as a hotline and text messaging service for pregnant women and caregivers for young children. The mobile phone service helps reduce unnecessary trips to hospitals and clinics, which is especially useful for families living in remote areas of the country. Parents can call in with symptoms and will be referred to the hospital if they are serious. Expecting mothers and young families also receive timely health information and advice based on the week of pregnancy or a child’s age. In 2017, Chipatala Cha Pa Foni was taken on by the Malawi Ministry of Health and made available nationwide.
India: Male Health Activists
Building on existing networks of female community health workers, this initiative added a male component with Male Health Activists. MHAs engaged the men who were household decision-makers and advocated for the importance of overall healthy habits and especially the maternal healthcare services that their wives needed (and the pediatric services that their children would eventually need). This helped women who may want access to maternal healthcare but were prohibited from traveling or leaving the house for checkups to fight the barrier of harmful gender norms.
Sierra Leone: Helping Health Workers Cope and Quality Circles
Focusing on the well-being of those who cared for others, HHWC provided psychosocial support through both group and individual counseling sessions. These sessions helped health workers to better cope with the stress and pressures of their work, build self-care routines, and become better carers for their patients and clients.
Quality Circles was another initiative designed to support healthcare workers and traditional birth attendants by creating peer learning and support groups. Through sharing knowledge and developing joint problem-solving skills, they were able to become more active members of the health system, resolving gaps and failures while being more effective in their jobs.
Ghana: Community Health Nurses on the Go
CHN on the Go was a smartphone app designed for frontline nurses. The app offered point-of-care support, planning tools, professional development, and wellness content. As part of the Care Community Hub, nurses who were in rural community areas were connected via WhatsApp groups to their peers, mentors, and supervisors so that they could get feedback and solve problems in-the-moment with their patients.
Ghana: Community Benefits Health
This initiative used creative, non-monetary incentives along with social and behaviour change to cultivate community-level commitment to supporting women and improving maternal and child health. While everyone stands to gain from the incentive — such as a water pump or a community-run ambulance known as an emergency transport system — the incentives are particularly beneficial to pregnant women and new mothers. An emergency vehicle gets an expectant mother to a health center quickly, while a closer borehole solves the problem of mothers traveling long distances daily to collect water.
Kenya: The Maker Movement
A critical shortage of working medical equipment is one reason why so many women and babies cannot receive the health care services they need for a healthy pregnancy and childbirth, resulting in needless deaths. This innovative partnership between Kenyatta National Hospital’s maternity ward doctors, nurses, and biomedical engineers and the University of Nairobi’s engineers and students created low-cost, high-quality locally-designed devices for Kenya’s resource-strapped maternity wards.
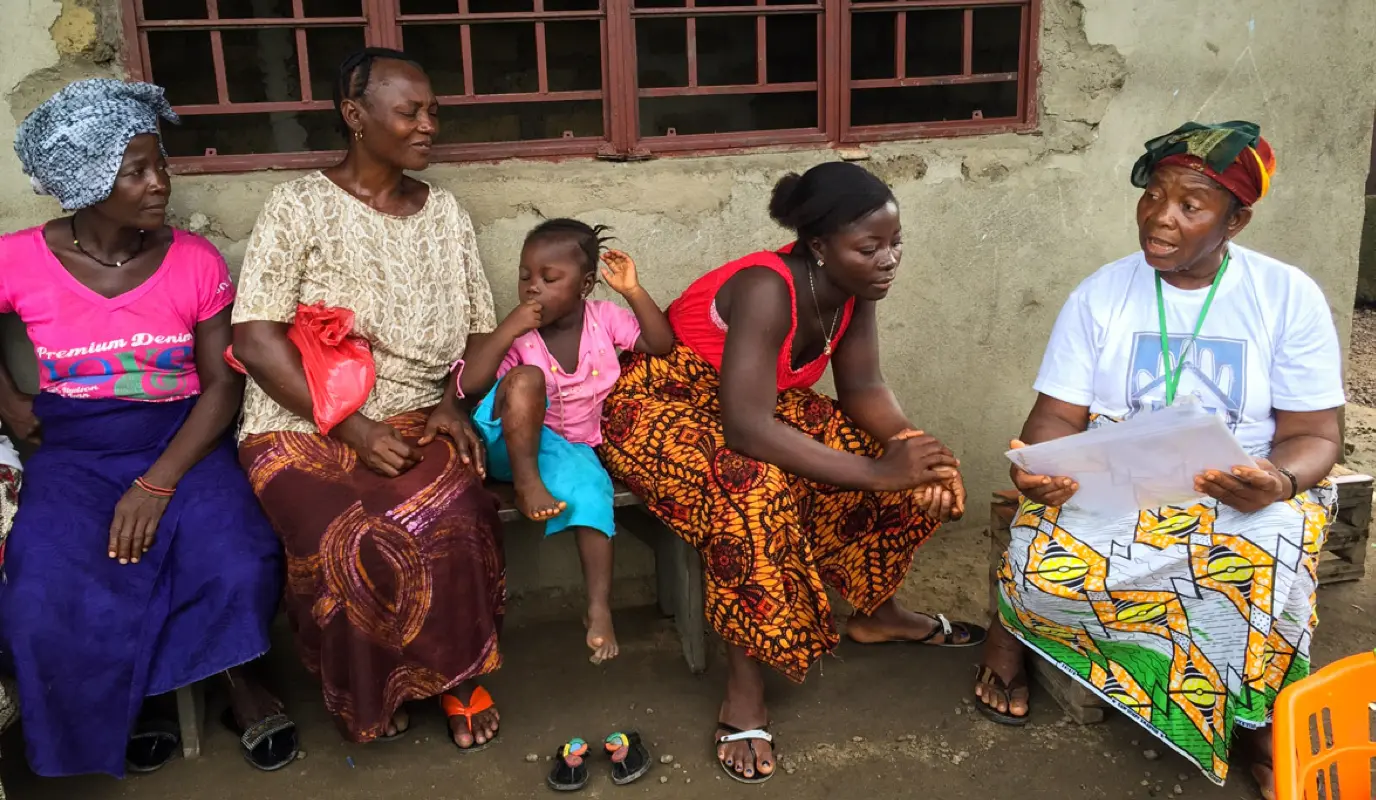
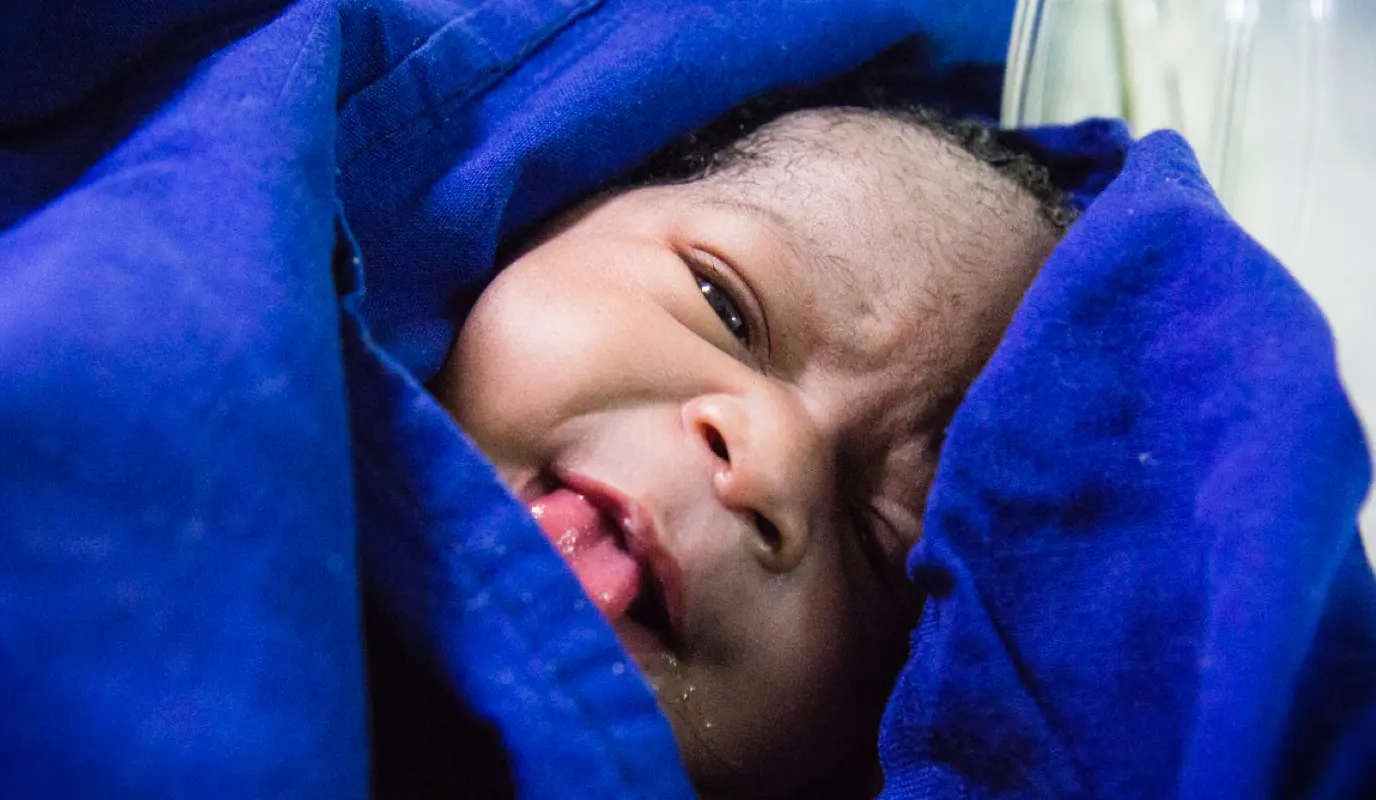
Sierra Leone: Essential Newborn Care Corps
In Sierra Leone, which has one of the world’s highest mortality rates for newborns and pregnant women, women historically gave birth at home with the help of a traditional birth attendant. Because TBAs had little (if any) formal healthcare training, the Sierra Leonean government made healthcare for pregnant women and young children free, and discouraged TBAs from facilitating home births. However, this change in routine was hard to make for expecting mothers, especially as clinics were often far away, short-staffed, and regarded with suspicion. Needless deaths continued. The Essential Newborn Care Corps flipped this problem by working with traditional birth attendants to give them the training, knowledge, and supplies they needed to give a quality of care to the women who relied on them. When this program was interrupted during the 2014-16 West African Ebola epidemic, we adapted this training to also include frontline Ebola support.
Kenya: Planwise
Using open-source big data and computer modeling, this tool helps planners in low-resource settings find the ideal locations for obstetric and prenatal care, as well as other health services. With PlanWise, planners can see the gaps and broken links (such as a shortage of clinics, or lack of transport) that stop women from being able to access timely emergency obstetric and newborn services. Armed with this information, leaders can then determine where best to build their next health facility, add ambulances, or deploy mobile clinics to ensure that mothers get the lifesaving care they need.
Your Support
Your tax-deductible gift makes you part of a vital community that enables us to reach nearly 10 million people each year with lifesaving health and nutrition solutions, fueled by authentic, empathic engagement and innovation. Your support can make it happen.
