How do we keep the “community” aspect of Community Management of Acute Malnutrition in an age of social distancing?
Hunger has been a reality in South Sudan longer than South Sudan has been an independent country. A decade of conflict, climate change, economic crisis, and scarce resources has led to 7.2 million people (more than 64% of the population) facing a hunger crisis. Of those 7.2 million, nearly one in five are children. Many of these children have grown up in Protection of Civilian (POC) sites, temporary tent shelters that were designed to accommodate a few days worth of displacement, but have since become semi-permanent homes for hundreds of thousands of South Sudanese fleeing violence in their communities.
Part of Concern’s work in South Sudan since the beginning was to provide lifesaving nutritional support for the millions of children facing severe acute malnutrition. In the Northern Bar el Ghazal state, our Community Management of Acute Malnutrition (CMAM) program supports children ages five and younger — as well as pregnant and lactating mothers — to ensure that they have all the resources they need for long, healthy, creative lives. Four of our 72 nutrition sites are specifically located in POC sites to cater to the added challenges of displacement.
Then COVID-19 happened.

Triaging healthcare in a crisis
When Concern co-piloted the program that would become CMAM a little over 20 years ago, one of the main challenges we wanted to address in the previous standard for treating malnutrition was finding a way to care for children at home.
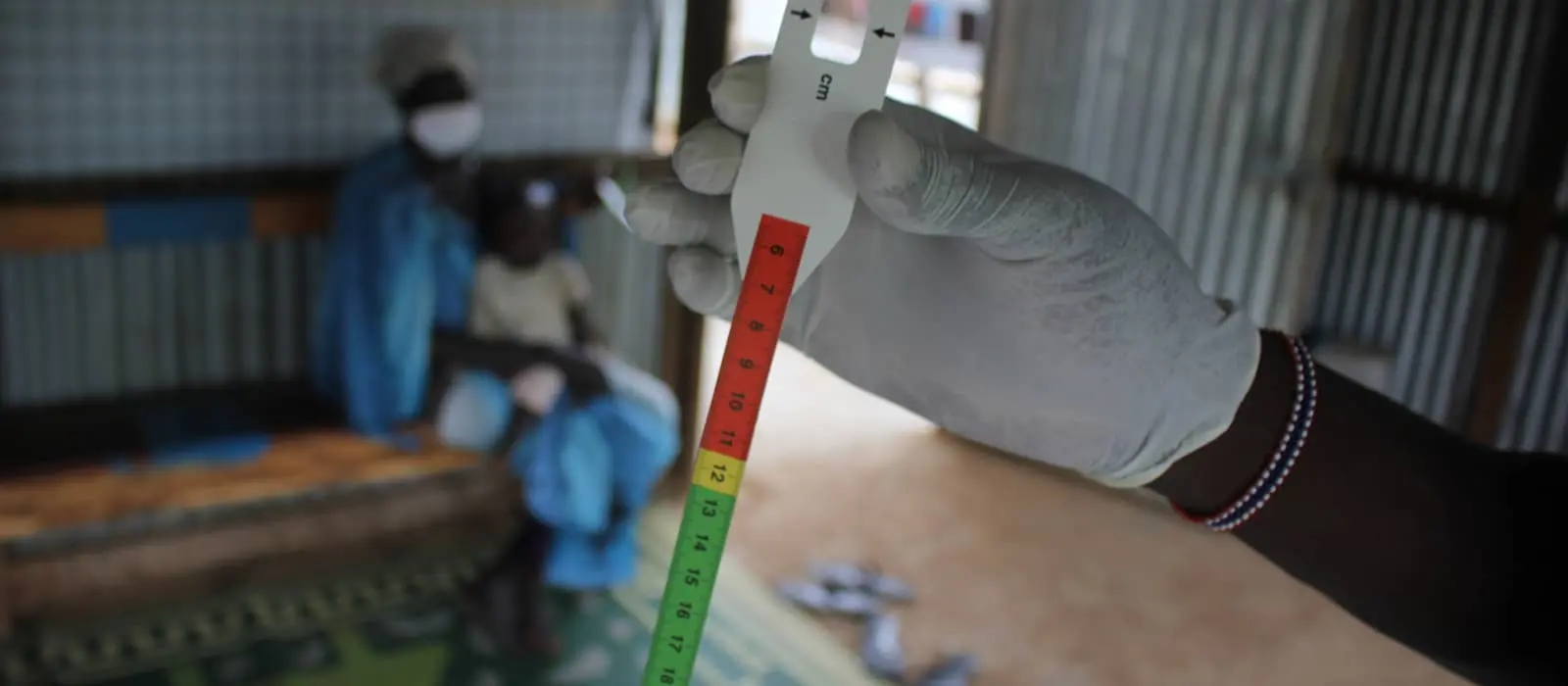
CMAM meant that children could easily be screened by community healthcare workers; using mid-upper-arm circumference (MUAC) was a great alternative to weighing a child in order to diagnose malnutrition. Ready-to-use therapeutic food (RUTF) made out of a shelf-stable peanut paste meant that parents could keep a course of treatment at home without needing to worry about contamination or refrigeration.
But we still needed our community healthcare workers to make contact with caregivers and children in screening for and treating acute malnutrition. The need for social distancing in order to curb the spread of COVID-19 made this part of the program a challenge, the bitter irony being that, in order to treat one public health crisis, we were faced with the threat of allowing another public health crisis to go unchecked.

Lockdown's ripple effect
Social distancing is integral to curbing the spread of a virus like COVID-19, however in many countries — South Sudan included — the greater impact was not the number of cases of COVID, but rather the ripple effect of not going out.
Arek Atak is a 65-year-old grandmother in Northern Bahr el Ghazal. Before the pandemic, she joined other women in her village in the nearby forest to collect firewood. The income she made from selling that at her local market, as well as some additional work weeding farmer’s plots of land during planting season, supported her family, including her 18-month-old granddaughter, Abuk.
Arek’s firewood group stopped meeting after the coronavirus was first diagnosed in South Sudan in April, 2020, and none of the women felt comfortable going by themselves to collect wood. Her other work also dried up as many of her clients did not cultivate crops due to delayed rains, lack of resources to plant, and not enough money.
The income was enough to keep things going, but without much savings to fall back on and with all of her friends and relatives suffering similar financial setbacks, there wasn’t much of an option. Three months into the pandemic, she sold her remaining two goats in order to purchase a month’s worth of food. She foraged wild fruits and vegetables when inflation quadrupled the price of staples like sorghum. Unfortunately for Abuk, none of these coping mechanisms were enough to offset the first signs of malnutrition.

Nimble by nature
Shortly before Abuk came to one of Concern’s nutrition centers, and in keeping with guidance from a consortia of organizations working in South Sudan (including the International Medical Corps, UNICEF, the World Food Program, and Action Against Hunger), we began to adapt our nutrition programs in order to fight both hunger and COVID-19 in South Sudan.
In addition to what are now familiar sights like increased handwashing facilities, supplies of hand sanitizer, temperature checks at entrances to our nutrition facilities, and markers to keep patients six feet apart, we focused on four key changes:
- Changing the admission criteria for CMAM
- Changing the dosage of RUTF during malnutrition treatment
- Changing the number of follow-up appointments during treatment
- Suspending mass screenings and helping families learn to screen their own children
The beauty of a program like CMAM is that it already works to bring the management of childhood malnutrition back home to communities, rather than forcing parents to bring their children to treatment centers that may be days away on foot and, in conflict settings, were prone to attacks. Adapting even more to the current challenges is part of CMAM’s DNA, and one of the reasons that making these adjustments was possible.
Keeping the doors open
When Concern admits a patient to CMAM, we look at three basic criteria: nutritional edema (diagnosed by pressing a child’s feet), MUAC, and their weight relative to height.
To keep with social distancing practices, weighing children at our nutrition centers was suspended. For a child like Abuk, this is good data to have, but not strictly necessary to diagnose malnutrition: By June 2020, she had a fever, diarrhea, and some visible signs of wasting. For an 18-month-old girl, an ideal mid-upper-arm circumference would be somewhere around five and a half inches. Abuk’s was just over four inches, placing her in a red zone.
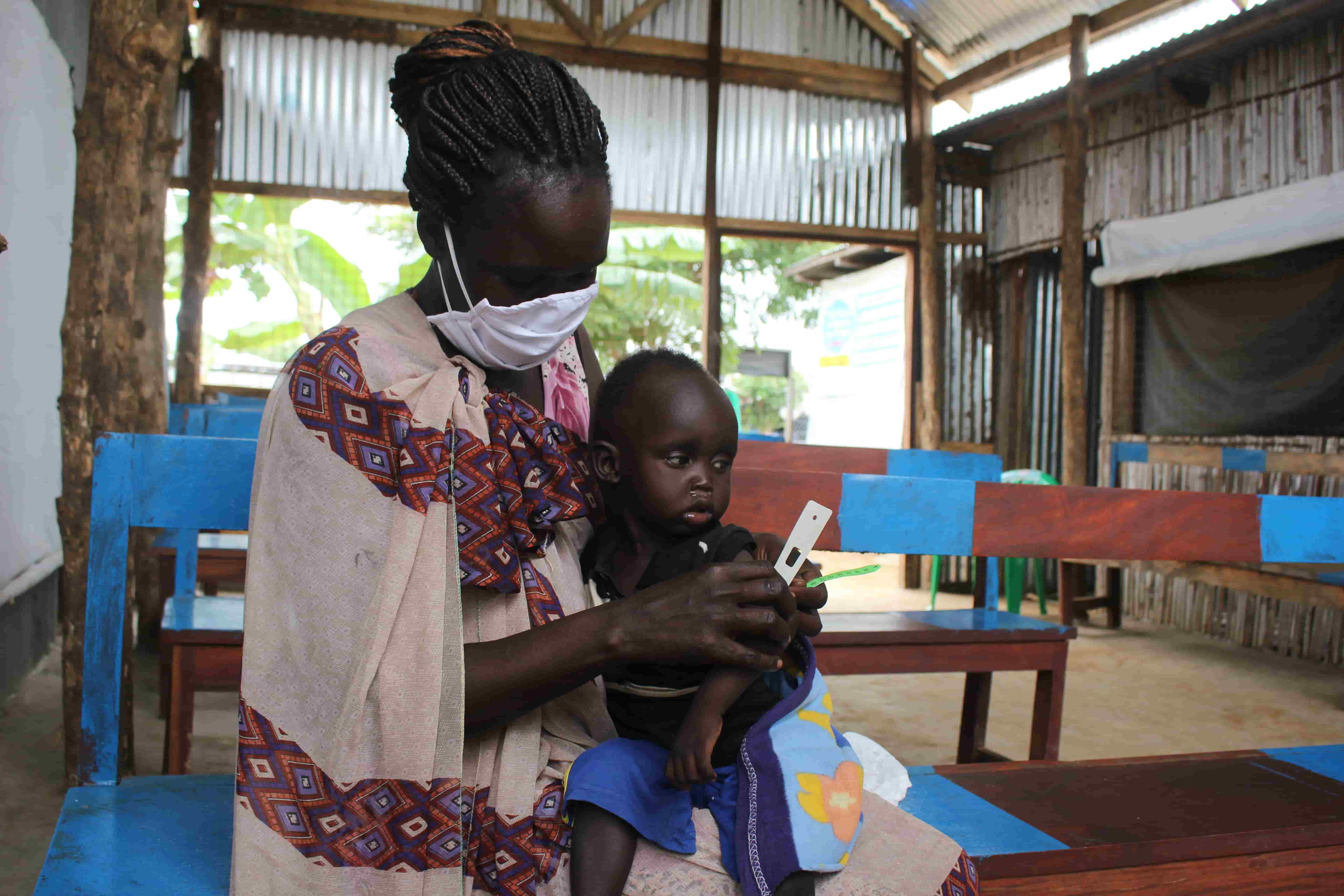
Suspending weight and height measurements at Concern’s nutrition sites in South Sudan minimized contact between staff and children. With MUAC measurements being a strong indicator of malnutrition, nutrition staff also trained parents and caregivers in how to use their own MUAC tape at home to measure their child’s progress and reduce further contact. After noticing a decline in CMAM participants, Concern expanded the program by distributing MUAC tape to caregivers in the community with children under five. Community nutrition volunteers trained caregivers and gave them information on what to do next if they noticed that their child was showing symptoms.
Continuing treatment
RUTF doses for outpatients are traditionally calculated based on a child’s weight. Based on both the mandate to reduce contact (including weighing children), and recent independent data in South Sudan, Concern also used a simplified protocol for treatment: Every child received two sachets per day, regardless of weight.
The modified dosage reduced demand on nutrition supplies within our clinics, made stock management easier, and allowed nutrition clinic staff to calculate rations more quickly. To date, cure rates for malnutrition in Concern South Sudan’s programs continue to be above standard, and most children enrolled in CMAM continue to grow.
Based on the national guidance, Concern also reduced the frequency of scheduled follow-up visits for children in the program. Abuk’s diagnosis of severe acute malnutrition would have normally kept her back at Concern’s nutrition center for weekly visits (more moderate cases of acute malnutrition were seen every other week). In order to reduce the number of in-person visits, severe cases were moved to biweekly visits, and moderate cases came back once a month. Caregivers were also given specific days for their appointments, versus walk-ins, and nutrition sites added more hours for these visits to accommodate the new schedule.
How did we do?
All of these steps successfully reduced crowding at nutrition centers without dramatically compromising the quality of care that CMAM offers (although treatment times increased, on average, by a week; likely due to a combination of pandemic-related factors). In addition to guidance from our local nutrition consortium, Concern had previous experience with site setups and family MUAC trainings, which made these modifications easier to roll out.
Concern’s focus on hiring nutrition staff from within communities also helped keep quality care going on-the-ground, even when access was restricted due to lockdowns. The change in our screening process also gave our nutrition teams more time to work in the community teaching families how to use MUAC tape, following up on individual cases, and conducting activities related to COVID awareness.
Abuk was one success of the program. When we last checked in with her and grandmother Arek, she had transitioned from outpatient therapy to supplemental therapy, and has been heading in the right direction in terms of her health and nutrition.
It’s not a perfect system, and it’s not a long-term solution. Arek told us she still worries about the uncertainties that lie ahead as COVID continues to change and have the harshest effects on the most vulnerable communities. Still, it’s one way we can continue to adapt to unpredictable times and ensure that they don’t leave those struggling to keep up even further behind.
Concern in South Sudan
Concern has been in South Sudan longer than the country has existed. Our recent work in the country has included:
- Providing lifesaving emergency nutrition and health services provided to acutely malnourished children and women, reaching over 142,000 people via 78 nutrition centers.
- Consulting and treating more than 68,000 children and mothers via our mobile clinics in five hard-to-reach areas in Aweil North and West counties, which also provided nutrition sessions for over 90,000.
- Reaching over 150,000 people in Unity State and Northern Bahr el Ghazal, including 34,000 people living in Bentiu displacement camp with water, sanitation, and hygiene interventions.
- Delivering nutrition support and sufficiency to 19,000 people who took part in cash-for-work activities and were also supported with hand tools and improved staple crop seeds.
- Improving water access for 49,000 people as a direct response to COVID-19.
However, this work is also under threat due to funding cuts. Your support of Concern — especially as a monthly donor — can help fill vital gaps left by large-scale donors, with $0.93 of every dollar going directly into our programs.